What is Pneumococcal Disease?
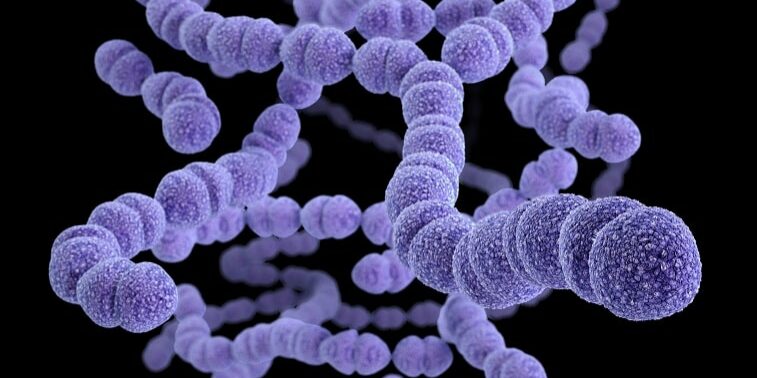
Pneumococcal (noo-muh-KOK-uhl) disease is caused by bacteria (Streptococcus pneumoniae) that can infect different parts of the body.
These bacteria (pneumococci) can cause common conditions like middle-ear infection (otitis media) and sinusitis.
These bacteria can also cause more serious conditions. When they invade the lungs, they can cause pneumonia; when they invade the bloodstream, they can cause bacteremia (that can lead to sepsis); and when they invade the lining of the brain, they can cause meningitis. These serious conditions often require hospitalization and can lead to death.
Who is at Risk?
Anyone can get pneumococcal disease, but some groups are at increased risk including:
- Young children
- Older adults
- Children and adults with certain chronic health conditions, including chronic heart disease, lung disease, kidney or liver disease, diabetes, sickle cell disease, or illnesses that weaken the immune system, such as HIV and certain cancers, among others
Pneumococcal disease is spread from person to person through coughing, sneezing, and close contact. Some people, especially children, can carry the bacteria in their nose and throat without being sick and can spread the bacteria to others.
How Serious is Pneumococcal Disease?
Pneumococcal pneumonia is a leading bacterial cause of hospitalized pneumonia in the US. Older adults and people with certain health conditions or other risk factors are at increased risk of serious outcomes or death from pneumococcal pneumonia.
Fewer adults get pneumococcal meningitis or bloodstream infection (bacteremia), but the mortality rate for these infections is high. Pneumococcal meningitis kills about 1 in 6 older patients who are infected and bacteremia kills about 1 in 8 adults who are infected. Both conditions can also result in lifelong disability including deafness, brain damage, and limb amputation.
Symptoms
People with serious pneumococcal infections may have a combination of high fever, chills, cough, shortness of breath, chest pain, stiff neck, disorientation, and sensitivity to light. The specific symptoms of pneumococcal infection depend on the part of the body affected (lungs, brain or spinal cord, or blood). Pneumococcal infections can affect multiple body areas and/or systems at the same time. Early diagnosis and treatment are very important for serious pneumococcal infections.
Prevention
Vaccination is the best way to protect against pneumococcal disease. Pneumococcal vaccination is recommended for:
- All children younger than age 5 years
- All adults age 50 years and older
- Individuals with certain chronic health conditions or other risk factors
In the US, there are 2 types of pneumococcal vaccines (conjugate and polysaccharide) currently available. There are several pneumococcal conjugate vaccines (PCV15, PCV20, and PCVV21 [for adults only]). There is 1 pneumococcal polysaccharide vaccine (PPSV23). Vaccine recommendations vary by age and risk group. Many at-risk adults have not been vaccinated against pneumococcal disease.
Talk with a healthcare professional about pneumococcal vaccination.
Pneumococcal Vaccine and Flu Vaccine
Having influenza (flu) increases the risk of getting pneumococcal disease so protection against pneumococcal disease is especially important during flu season. If both vaccines are due, they can be given during the same visit for both children and adults, but they should be given in 2 different injection sites (for example, different arms or at least 1 inch apart if in the same arm).
Pneumococcal Vaccine and COVID-19 Vaccine
COVID-19 vaccines can be given on the same day as pneumococcal vaccines, but each vaccine should be injected in a different site (for example, different arms or at least 1 inch apart if in the same arm).
Treatment
Antibiotics are used to treat pneumococcal disease. However, pneumococcal bacteria can be resistant to antibiotics commonly used for treatment. In serious infections, treatment may start with a broad-spectrum antibiotic, which works against a wide range of bacteria. After testing, once more is known about the specific bacteria the patient has, a more targeted antibiotic may be selected.
Updated November 2025
Sources: American Academy of Family Physicians, American Academy of Pediatrics, Centers for Disease Control and Prevention
Key Audiences
Related Resources

Dan’s Story (Pneumonia)
Dan has a chronic health condition. This makes him more likely to get pneumonia. A vaccine may have saved his life.

Respiratory Immunization Updates: Protecting Maternal and Special Populations
In this recorded webinar, NFID hosts a discussion on the importance of respiratory vaccination among pregnant women and immunocompromised individuals …

2025 National Survey on Respiratory Diseases
The 2025 national survey examines attitudes and behaviors regarding flu, RSV, COVID-19, and pneumococcal disease.
Related Posts

Advancing Prevention in a Complex Respiratory Season
2025–2026 Respiratory Campaign round-up: NFID and partners urge immunization to help protect against COVID-19, flu, RSV, and pneumococcal disease
5 Reasons Why Vaccines Are Good for Your Heart
For people with heart disease, getting vaccinated is as important to staying healthy as diet and exercise

NFID Calls for Evidence-Based Guidance as Many People Skip Life-Saving Respiratory Vaccines
Survey reveals misconceptions about vaccines and declining vaccination rates



