Some people have health problems that last months or even years after they are infected with the virus that causes COVID-19. If these symptoms last for three months or more, healthcare professionals call it post-COVID conditions (PCC) or Long COVID.
Dozens or even hundreds of symptoms may fall under the description of Long COVID. The symptoms vary widely from person to person. Nearly any organ in the body can be affected.
Long COVID is a new condition, and scientists still have a lot to learn about it. Studies are underway to learn more, but it will take time to find answers. Information is likely to change as researchers learn more.
How Common or Serious is Long COVID?
Around 5-8% of people who have COVID-19 develop Long COVID. Fewer people are developing Long COVID today compared to early in the pandemic. That’s partly because the virus has changed to become less likely to cause serious disease. But it’s also because more people are vaccinated.
Long COVID can involve mild symptoms that take a long time to go away. But for some people, it can be serious enough to limit daily life for months or years.
What Causes Long COVID?
Researchers have not found a single cause of Long COVID. There may be more than one. Some of the possibilities include:
- The virus remains in the body
- The immune system starts attacking the body’s own cells, or it may not be working in other ways
- Microbes in the gut get out of balance, affecting how the body produces energy or how the gut and the brain communicate with each other
- Damage to cells in the blood vessels triggers clots
- Effects on energy-producing parts of cells called mitochondria
- COVID-19 may wake up other viruses hidden in the body
Who is Most at Risk for Long COVID?
Anyone who had COVID-19 can develop Long COVID, but the condition is more common in people who:
- Had more serious COVID-19 illness, especially those who were hospitalized
- Have not been vaccinated against COVID-19
- Have health conditions like diabetes, heart disease, or high blood pressure (hypertension)
Women are more likely than men to develop Long COVID.
People who have difficulty accessing healthcare, communities of color, and people with disabilities may be at greater risk for developing Long COVID.
Symptoms: What Does Long COVID Feel Like?
Long COVID can include a wide range of symptoms. Some of the most common are:
- Loss of smell or taste
- Trouble concentrating or remembering (“brain fog”)
- Feeling very tired
- Headaches
- Feeling dizzy or lightheaded
- Racing heartbeat
- Long-lasting cough
- Trouble catching your breath
- Diarrhea, constipation, or bloating
- Worsening symptoms after minor physical or mental activity
This is not a complete list. Long COVID may be responsible for hundreds of possible symptoms. They may linger after the original infection, or they may appear later. They may go away and come back again. In some people, COVID-19 triggers new health conditions.
How Can Long COVID Be Prevented?
Since Long COVID can develop after every COVID-19 infection, preventing COVID-19 is the best way to avoid Long COVID.
Stay up to date on vaccination, even if you have already been vaccinated. COVID-19 vaccines are updated to keep up with the changing virus.
The best way to prevent long COVID is to protect yourself and others from being infected:
- Get vaccinated against COVID-19
- Get tested for COVID-19 as needed
- Get treated for COVID-19 if recommended by a healthcare professional
- Practice healthy habits to help prevent the spread of COVID-19:
- Wear a face mask as recommended
- Wash your hands with soap and water for at least 20 seconds
- Avoid touching your eyes, nose, and mouth
- Cover coughs and sneezes with a tissue
- Avoid close contact with people who are sick and stay home if you are sick
How is Long COVID Treated?
There is no specific test, treatment, or cure for Long COVID. Because Long COVID takes many different forms, treatment varies from person to person.
Talk with a healthcare professional about when symptoms first started, how often they occur, what makes them worse, and how they affect daily activities. Your healthcare professional can help you develop a personal plan to treat symptoms and improve quality of life.
Updated and reviewed May 2026
Sources: Centers for Disease Control and Prevention, National Academies
Related Resources
What Is an Antiviral?
Overview of antivirals—what they are, how they work, and what diseases they help treat

Don’t Be A Dreaded Spreader
In this episode, NFID experts offer insights on updated recommendations from the Centers for Disease Control and Prevention (CDC) to help prevent the spread of respiratory viruses, including COVID-19, influenza (flu), and respiratory syncytial virus (RSV)
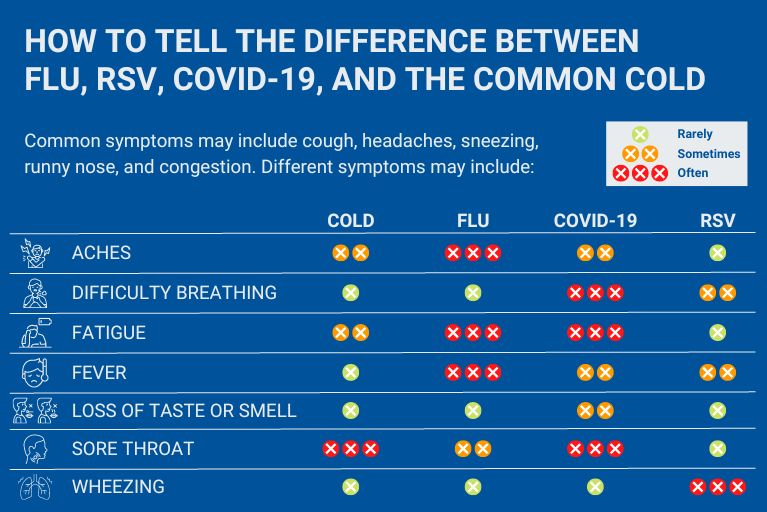
How to Tell the Difference between Flu, RSV, COVID-19, and the Common Cold
Graphic listing common symptoms of respiratory viruses
