Special thanks to Kenneth E. Schmader, MD, Professor of Medicine, Chief of Division of Geriatrics at Duke University Medical Center, Director of Geriatric Research, Education, Director of the Clinical Center at the Durham VA Medical Center, and NFID Clinical Vaccinology Course faculty member, for this guest blog post on the importance of shingles prevention.
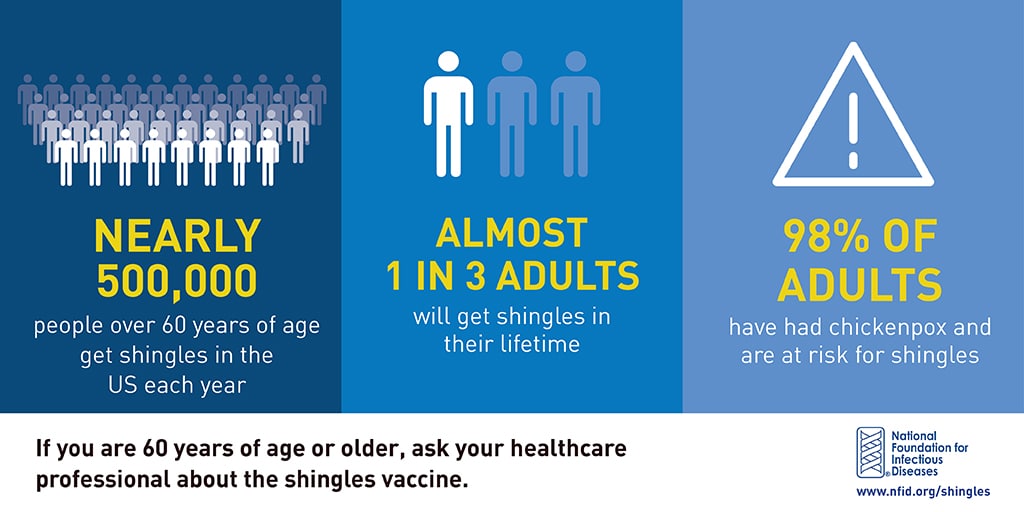
Almost 1 in 3 people in the US will develop shingles during their lifetime and the risk of shingles increases with age. If you are 60 years of age or older and have not been vaccinated against shingles, you should ask a healthcare professional about shingles vaccination.
What is shingles?
Shingles (herpes zoster) is caused by the varicella zoster virus—the same virus that causes chickenpox. The virus stays inactive in the body for life and can reactivate years, or even decades, later causing shingles. Shingles causes a painful, blistering skin rash that can last 2-4 weeks. Shingles can be treated with antiviral and pain medication but for some individuals, the pain can last for months, or even years, after the rash goes away. This pain is called postherpetic neuralgia (PHN) and is the most common complication of shingles. Pain from shingles has been described as excruciating, aching, burning, or stabbing and the risk of PHN increases with age. Other complications may include skin infections, eye problems, and muscle weakness.
What is my risk of getting shingles?
About one million shingles cases occur in the US every year and almost one in three US adults will get shingles in their lifetime. Risk increases with age—shingles is 10 times more likely to occur in adults age 60 years and older than in children under 10 years old. Shingles is associated with normal aging and anything that weakens the immune system such as certain medications, cancers, or infections, but it can also occur in healthy children and younger adults.
What are the symptoms of shingles?
The first sign of shingles is often a burning or tingling pain or itch, generally in a band-like distribution on one side of the body (around the waist, chest, stomach, or back) which can be mild or intense. The second sign is a rash of fluid-filled blisters similar to chickenpox but they typically occur in a cluster rather than scattered over the body. In some cases, blisters may also occur on one side of the face around the eye and on the forehead.
Is shingles contagious?
Shingles cannot be passed from one person to another. However, a person with shingles can transmit varicella zoster virus to others. An individual who gets infected with varicella zoster virus for the first time will develop chickenpox, not shingles.
How can you reduce your risk of getting shingles?
Fortunately, there is a safe and effective vaccine that can reduce your chances of getting shingles. The vaccine is recommended for individuals age 60 years and older, however certain individuals such as those with a weakened immune system may have to wait to get vaccinated, or should not get vaccinated at all.
Take this quick quiz and talk to a healthcare professional to find out if the shingles vaccine is right for you.
Can I get vaccinated if I have already had shingles?
Most people who get shingles will have it only once, but a recurrence is possible. Even if you have had shingles, you can still receive a shingles vaccine to help prevent future occurrences of the disease. There is no specific length of time you must wait after having shingles before receiving a shingles vaccine, but you should make sure the shingles rash has disappeared before getting vaccinated. Some experts recommend waiting at least a year after the onset of the shingles rash before receiving the vaccine.
Visit adultvaccination.org/shingles to learn more about shingles and its prevention.
To join the conversation, follow NFID on Twitter (@nfidvaccines), like NFID on Facebook, join the NFID Linkedin Group, and subscribe to NFID Updates.
Related Posts
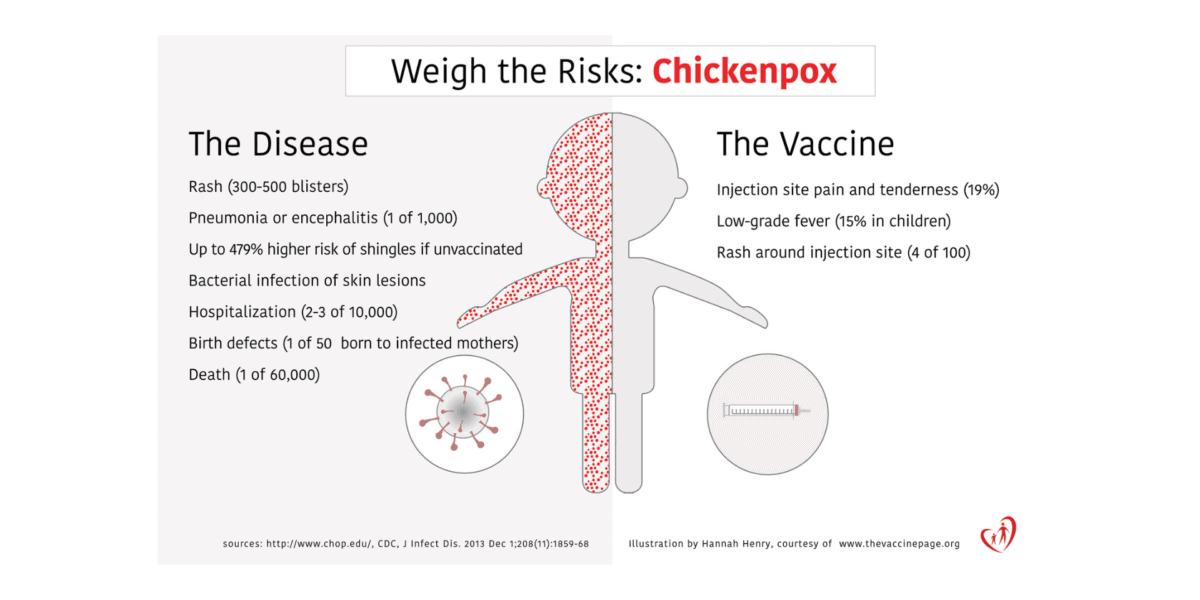
Spread Information, Not Diseases
Vaccines are among the most significant achievements in public health and can help protect against 14 deadly diseases. Share these infographics to help spread information, not disease!

Developing Improved Vaccines for Older Adults
By 2030, the number of adults age 65 years and older in the United States is expected to grow to 71 million—at least 20 percent of the total population. It is particularly important during this stage of life to maintain healthy lifestyles and habits. Receiving recommended immunizations is an essential part of that process.,,

A Heart Healthy Lifestyle Includes Adult Vaccines
Along with Valentine’s Day, February is also American Heart Month, a great time to commit to a healthy lifestyle and make small changes that can lead to a lifetime of heart health. NFID reminds those with heart disease to stay up-to-date on all recommended vaccines, especially flu, pneumococcal, Tdap, and shingles…